Treatments
for Multiple Myeloma
As a multiple myeloma patient, it's important to start the right treatment plan quickly to increase your chances of achieving your best outcome.
Determining the Right Treatment Plan
Treatment Approaches
by Multiple Myeloma Stage
Goals of Multiple Myeloma Treatment
- Reduce the amount of M protein (as measured by serum protein electrophoresis) or light chains (as measured via the free light chain test) to the lowest level possible
- Eliminate myeloma cells from the bone marrow (as measured via minimal residual disease [MRD] testing)
- Improve quality of life with as few treatment side effects as possible
- Provide the longest possible period of response before first relapse
- Prolong overall survival
Treatment of Newly Diagnosed Multiple Myeloma
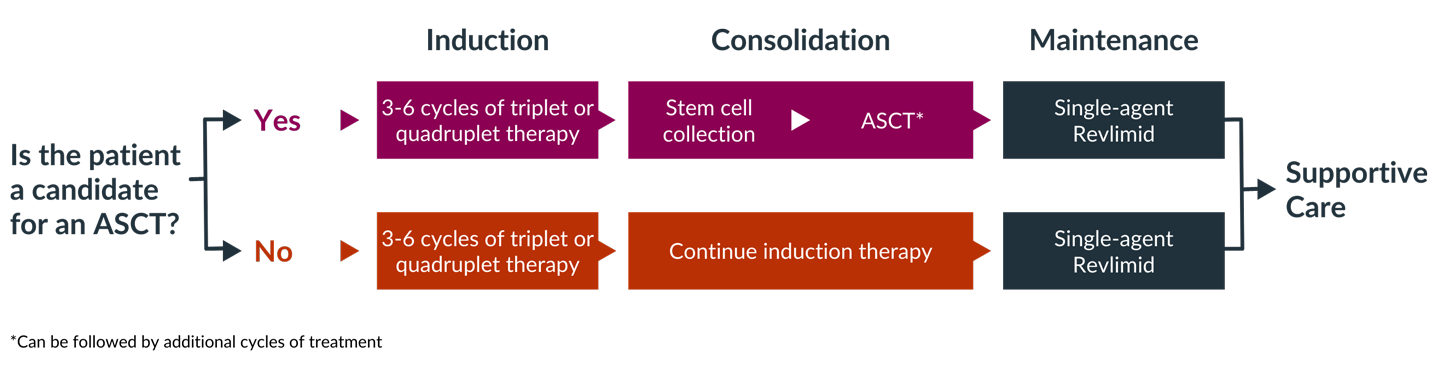
Induction therapy
Induction therapy, or front-line therapy, typically consists of a three-drug or four-drug combination regimen given over three to four cycles, each of which typically lasts 3 or 4 weeks.
Three-drug regimens (triplet therapy) generally include an immunomodulatory drug (Revlimid or Pomalyst), a proteasome inhibitor (Velcade, Kyprolis, or Ninlaro), and a steroid (dexamethasone or, less commonly, prednisone).
Four-drug regimens (quadruplet therapy) are similar to three-drug regimens but also include an anti-CD38 monoclonal antibody (Darzalex or Sarclisa).
The choice of initial treatment depends on many factors. These include the features of your myeloma, the risk of side effects, convenience for you, and the familiarity of the doctor with the available treatment options.
One of the first questions that must be answered, by both you and your doctor, is whether you are a candidate for high-dose chemotherapy followed by an autologous stem cell transplant (ASCT). Determining whether transplant is an option is an important factor in selecting induction therapy. If you are a candidate for transplant, you may choose to have a transplant after three or four cycles of induction therapy or you may decide to complete induction therapy and consider transplant later.
If you are eligible and decide to proceed with a transplant, you will usually receive induction therapy followed by stem cell collection and storage, high-dose melphalan chemotherapy, and ASCT. This is then followed by consolidation and/or maintenance therapy. If you opt to delay ASCT, your stem cells would still be collected and stored for use in the future.
If you are not eligible for a transplant, you will go directly from induction therapy to consolidation or maintenance therapy, depending on your response to induction therapy.
Your care team can help decide which course of therapy is best for you, based on the characteristics of your myeloma, your treatment goals, and your personal situation.
Autologous stem cell transplant
Bone marrow transplants are no longer done in multiple myeloma. Instead, almost all transplants in multiple myeloma use cells obtained from the blood; these are referred to as peripheral blood stem cell transplants.
The main type of stem cell transplant performed for multiple myeloma patients is ASCT, which uses your own stem cells. Another type of transplant, allogeneic stem cell transplant, uses stem cells from a donor and is rarely used outside of clinical studies.
ASCT, in combination with high-dose chemotherapy (usually melphalan), is a treatment that, for many eligible myeloma patients, offers a very good chance for a long-lasting response. High-dose chemotherapy, though effective in killing myeloma cells, also destroys normal blood-forming cells (hematopoietic stem cells) in the bone marrow. Stem cell transplantation replaces these important cells.
Autologous stem cell transplantation steps
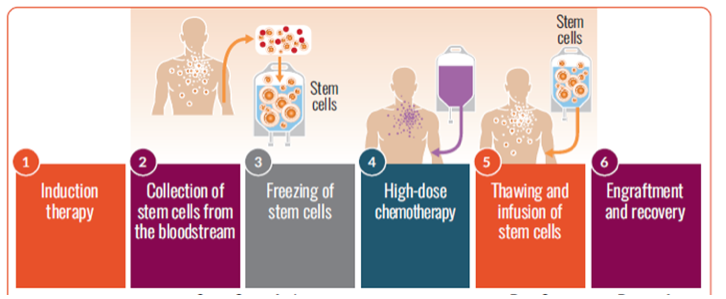
If you are eligible for a transplant, you are encouraged to have stem cells collected (harvested) so the cells are available if you choose to undergo transplantation at some point in the future.
The cells are stored until they are needed for the transplant. The stored stem cells are infused back into your blood. This procedure may be inpatient or outpatient, depending on the center and/or your preference.
Maintenance therapy
After induction and autologous stem cell transplant, you will undergo maintenance (continuous) therapy. Maintenance therapy is given after induction therapy to help keep the myeloma from growing back. Maintenance therapy improves survival and can increase the length of time you spend in remission, but it is also associated with treatment side effects.
Revlimid is an FDA-approved maintenance therapy option; Velcade and Ninlaro are also acceptable options, particularly if you cannot tolerate Revlimid. There are also several clinical studies looking at the effectiveness of different regimens for maintenance therapy, including Kyprolis, Darzalex, and Empliciti, alone and in combination with other treatments.
Treatment of newly diagnosed multiple myeloma
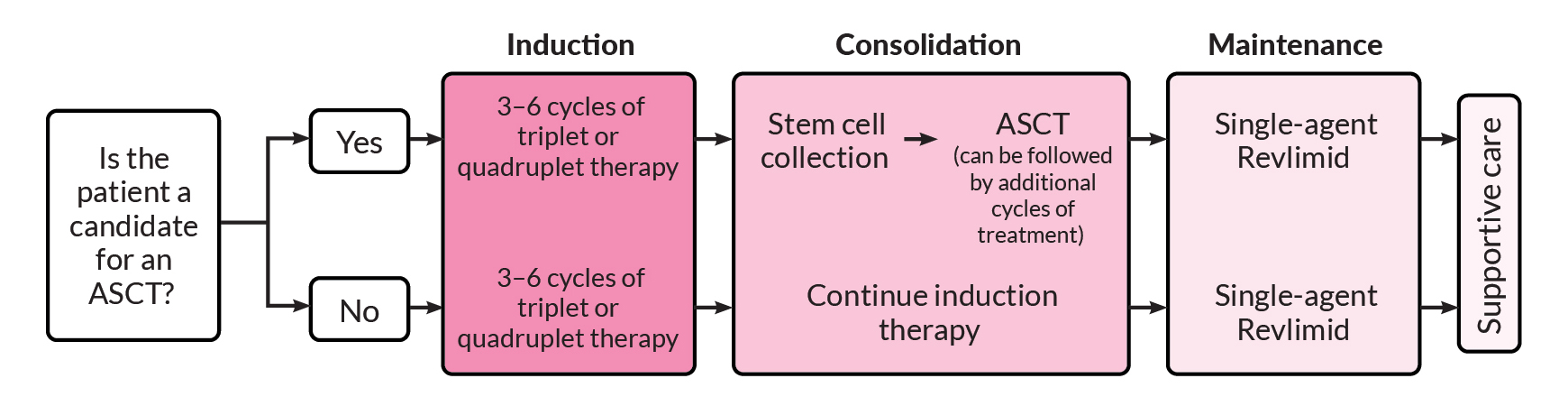
Relapsed/refractory multiple myeloma
If your multiple myeloma is resistant to therapy (refractory) or if your myeloma returns after an initial response to treatment (relapsed), you are said to have relapsed or refractory multiple myeloma.
There are many effective treatment options for relapsed myeloma—more are being tested in clinical studies—so if your myeloma relapses, you should not lose hope or think that there are no chances for an effective treatment.
Therapies for relapsed or refractory multiple myeloma are selected based on the number of prior myeloma treatments you have received and which treatments you already received (and may no longer work). Some treatments are used for patients who have had three or fewer treatments (who are said to be in early relapse), and different treatments tend to be used for patients who have received more than three prior therapies.
Therapies for early relapse
If you have early relapsed multiple myeloma, the treatment options include immunomodulatory drugs, proteasome inhibitors, and anti-CD38 monoclonal antibodies. This may include repeating the treatment used in your induction therapy or trying different therapies from the same class of treatment as those used for induction. In addition, drugs that work in new ways (novel mechanisms), like Xpovio (selinexor), may be used to treat early relapsed multiple myeloma. Combinations of these agents with dexamethasone are used to treat early relapse.
If your myeloma does not respond to immunomodulatory drugs, proteasome inhibitors, and anti-CD38 monoclonal antibodies, you are said to be triple-class refractory. Treatment options for triple-class refractory multiple myeloma have seen great advances in the last few years. In addition to novel treatments like Xpovio, therapies used to treat triple-class refractory myeloma include bispecific antibodies and CAR T-cell therapy.
Currently available treatments for patients with triple-class refractory disease:
Xpovio
Abecma
Carvykti
Tecvayli
Talvey
Elrexfio
If you have relapsed or refractory myeloma, there are new agents and therapies under investigation that may provide benefit. Your care team can help you find an appropriate study. You can also speak with an MMRF Patient Navigator for more information.
Standard Drug Therapies for Multiple Myeloma
Myeloma treatment can also involve what are referred to as supportive care therapies, which help in the management of myeloma symptoms and treatment side effects.
Proteasome inhibitors
Proteasome inhibitors are an important class of multiple myeloma treatments and are used at all stages of disease.
Three proteasome inhibitors are approved for use in multiple myeloma treatment: Velcade (bortezomib), Kyprolis (carfilzomib), and Ninlaro (ixazomib).
Velcade is typically given subcutaneously (under the skin) as a first-line myeloma treatment. It is also used as treatment if your myeloma has relapsed. Velcade is often given in combination with other drugs.
- Velcade is typically given for nine 6-week treatment cycles. When used as maintenance therapy, Velcade may be administered weekly or less frequently, such as once every 2 weeks, with similar or longer treatment periods.
- If you have reduced liver function (hepatic impairment), you will typically start with a reduced dose of Velcade. Depending on how you tolerate this dose, subsequent doses may be increased or decreased. The length of treatment with Velcade may be different for each patient and is based on how well the drug is working and if any side effects that develop are manageable. You and your doctor can discuss the length of treatment that may be right for you.
- If you are being treated with Velcade, your doctor may also give you medication to prevent shingles, a painful rash and is due to a reactivation of the virus that causes chickenpox.
- In 2022, a generic version of Velcade was approved by the FDA. In terms of safety, quality, performance characteristics, and intended use, generic Velcade is the same as the marketed brand-name drug manufactured by Takeda Oncology. Generic Velcade can be used as a substitute for Velcade.
- A common side effect of Velcade is peripheral neuropathy—that is, damage to the nerves in the hands and feet. The symptoms of peripheral neuropathy vary but are often described as pain, tingling (“pins and needles” sensation), burning, numbness, reduced sensation, trembling, tripping or stumbling when walking, difficulty in picking up small objects, and sensitivity to temperature. It often starts in the toes or fingers before moving inward to the ankles or wrists.
- If you experience peripheral neuropathy, your doctor will determine the best way to manage it based on the underlying cause, which could be the myeloma itself, a treatment you are receiving, or an unrelated condition you may have, such as diabetes.
Kyprolis is given intravenously (in a vein) and, like Velcade, can be used by itself or in combination with another drug. Kyprolis is used if you have previously received at least one other treatment for multiple myeloma. It can also be used as first-line therapy if you have higher-risk disease.
- Dosing varies depending on whether Kyprolis is given alone or in combination with other agents.
- Kyprolis is typically given twice weekly as a 10-minute or 30-minute infusion, depending on the dosing used. Kyprolis is given for 3 weeks on this schedule, followed by 12 days off.
- You may experience infusion reactions immediately following or up to 24 hours after receiving Kyprolis. These reactions can include fever, chills, achiness, flushing, facial swelling, vomiting, weakness, shortness of breath, low blood pressure, fainting, chest tightness, and chest pain. However, dexamethasone given prior to Kyprolis reduces the incidence and severity of these reactions.
- Kyprolis can also have cardiovascular side effects, including congestive heart failure. If you have a heart condition, you will be evaluated to determine whether Kyprolis is an appropriate treatment. If you have a heart problem and take Kyprolis, you will be monitored closely by your doctor.
Ninlaro is an oral drug that is given in combination with another drug if you have previously received another treatment for multiple myeloma. Ninlaro may also be used as first-line therapy when an oral therapy is preferable.
- The recommended starting dose of Ninlaro is 4 mg once a week on days 1, 8, and 15 of each 4-week cycle along with Revlimid and dexamethasone.
- If you have moderately or severely reduced liver function (hepatic impairment) or kidney function (renal impairment), or if you are receiving dialysis, you will typically receive a lower (3 mg) starting dose of Ninlaro.
- You should take Ninlaro with water once a week on the same day and at approximately the same time. You should take it at least 1 hour before or at least 2 hours after eating, separately from dexamethasone, which should be taken with food.
Immunomodulatory drugs
Immunomodulatory drugs are an important class of standard treatments used to treat multiple myeloma. They work by activating certain cells in the immune system, preventing myeloma cell growth, and even by directly killing myeloma cells.
The immunomodulatory drugs currently used to treat multiple myeloma include the oral agents Revlimid (lenalidomide), Pomalyst (pomalidomide), and, less commonly, Thalomid (thalidomide).
Revlimid, given in combination with dexamethasone, is used to treat all stages of multiple myeloma.
- Revlimid is administered orally.
- Dosing varies depending on whether Revlimid is given in combination with other agents or as maintenance therapy following ASCT.
- For newly diagnosed patients, Revlimid is typically administered on days 1–21 for each 28-day cycle.
- As maintenance therapy following ASCT, Revlimid is typically taken once daily for days 1–28 of repeated 28-day cycles, until relapse or until the patient experiences unacceptable toxicity. The dose may be increased if the starting dose was well tolerated for the first three cycles. If a patient experiences a sustained response, the dose may be reduced over time.
- Blood clots can occur when Revlimid and Pomalyst are used. The risk of clots is higher when these medications are used in combination with steroids (for example, dexamethasone). If you are newly diagnosed or have had blood clots in the past, you are at particularly high risk. Other risk factors for blood clots include older age, family history, other medical conditions, obesity, and long periods of sitting still or lying down.
- Your doctor will assess your risk of developing blood clots and may prescribe blood thinners to reduce the risk, such as aspirin or heparin. You can help prevent blood clots by avoiding long periods of inactivity.
- There have been reports of new second cancers (also called second primary malignancies or SPMs) developing in a small number of myeloma patients who received Revlimid therapy in clinical studies. Overall, the information available to date indicates that therapy with Revlimid significantly decreases the risk of myeloma disease progression. Most doctors believe that the benefits of Revlimid therapy outweigh any potential risk of second cancers.
- If you are pregnant or plan to become pregnant, you must not take immunomodulatory drugs. This precaution is due to some signs of birth defects in animals.
- In 2022, a generic version of Revlimid was approved by the Food and Drug Administration (FDA). In terms of safety, quality, performance characteristics, and intended use, generic Revlimid is the same as the marketed brand-name drug. Generic Revlimid can be used as a substitute for Revlimid.
Pomalyst is used if you have relapsed, refractory, or high-risk multiple myeloma or if you have kidney problems. It is more potent than Revlimid or Thalomid.
- Pomalyst is an oral medication that is taken along with dexamethasone.
- Typically, you will take aspirin or another blood thinner along with Pomalyst and low-dose dexamethasone.You will take Pomalyst and low-dose dexamethasone as long as they continue to work against the myeloma.
Thalomid is an older drug that has been used in combination with other drugs throughout all stages of multiple myeloma. With the development of newer drugs, Thalomid is used less often in myeloma treatment today in the United States.
- Possible side effects specific to immunomodulatory drugs
- Blood clots can occur when Revlimid and Pomalyst are used. The risk of clots is higher when these medications are used in combination with steroids (for example, dexamethasone). If you are newly diagnosed or have had blood clots in the past, you are at particularly high risk. Other risk factors for blood clots include older age, family history, other medical conditions, obesity, and long periods of sitting still or lying down.
- Your doctor will assess your risk of developing blood clots and may prescribe blood thinners to reduce the risk, such as aspirin or heparin. You can help prevent blood clots by avoiding long periods of inactivity.
- There have been reports of new second cancers (also called second primary malignancies or SPMs) developing in a small number of myeloma patients who received Revlimid therapy in clinical studies. Overall, the information available to date indicates that therapy with Revlimid significantly decreases the risk of myeloma disease progression. Most doctors believe that the benefits of Revlimid therapy outweigh any potential risk of second cancers.
- If you are pregnant or plan to become pregnant, you must not take immunomodulatory drugs. This precaution is due to some signs of birth defects in animals.
Monoclonal antibodies
Monoclonal antibodies are agents that fight disease by activating your immune system. These drugs enhance the cancer-fighting abilities of your own immune system by targeting multiple myeloma cells.
Currently, the most commonly used antibodies are Empliciti (elotuzumab), Darzalex (daratumumab), and Sarclisa (isatuximab).
- Empliciti is typically given as an intravenous (IV) infusion once a week for the first two cycles and every 2 weeks thereafter. Starting with the third cycle, infusions are given every 4 weeks.
- Before beginning treatment with Empliciti, you will receive dexamethasone, antihistamines, and a fever-reducing agent (acetaminophen) to reduce the risk of infusion reactions, which can occur following administration of Empliciti.
- Darzalex can be given either intravenously or subcutaneously. Darzalex Faspro is the subcutaneous (injection) formulation. This is the most commonly used and convenient administration for patients.
- For newly diagnosed patients, Darzalex/Darzalex Faspro, is given as part of a 3-drug (triplet) or 4-drug (quadruplet) combination therapy.
- Darzalex is administered intravenously weekly during weeks 1 through 8, every 2 weeks during weeks 9 to 16, and then every 2 weeks for 8 weeks.
- When used in combination with other drugs for relapsed or refractory multiple myeloma, Darzalex is typically administered weekly during weeks 1 through 8, every 2 weeks during weeks 9 through 24, and then every 4 weeks until disease progression.
- Darzalex Faspro is administered over approximately 3 to 5 minutes. The frequency of treatment is typically weekly during weeks 1 through 8, every 2 weeks during weeks 9 to 24, and every 4 weeks until disease progression.
- Before receiving Darzalex/Darzalex Faspro, you will be given antihistamines, fever-reducing agents, and steroids to reduce the risk of infusion reactions. Following the infusion or injection of Darzalex/Darzalex Faspro, you will also receive a steroid to reduce the risk of delayed infusion reactions.
- If you receive Darzalex/Darzalex Faspro, you will also be given antiviral medication to prevent shingles.
- Sarclisa is administered as an IV infusion given along with dexamethasone every week of a 28-day cycle. In subsequent cycles, Sarclisa is only administered every 2 weeks. The combination of drugs is continued until the disease progresses or you experience unacceptable side effects.
Bispecific antibodies
Bispecific antibodies are another type of antibody-based immunotherapy. There are currently four bispecific antibody therapies FDA-approved for myeloma patients who have received at least four prior lines of therapy: Tecvayli (teclistamab), Talvey (talquetamab), Elrexfio (elranatamab), and Lynozific (linvoseltamab).
- Tecvayli (teclistamab) is the first BCMA-targeted bispecific antibody approved for use as a myeloma treatment. It is given subcutaneously.
- Tecvayli is given in two step-up doses on day 1 and day 4, followed by the first treatment on day 7. Tecvayli is given once weekly thereafter until disease progression. If patients achieve and maintain a complete response (or better) for at least 6 months on Tecvayli, it may be given once every two weeks.
- Approximately 1 to 3 hours before each Tecvayli step-up dose, you will receive steroids, antihistamines, and acetaminophen. Because of the risk of side effects, you may be hospitalized for 48 hours after administration of each dose in the Tecvayli step-up dosing schedule.
- Side effects of Tecvayli may include cytokine release syndrome and neurologic toxicities.
- Talvey (talquetamab) is the first GPRC5D-targeted bispecific antibody approved for use as a myeloma treatment. It is given subcutaneously.
- For weekly dosing: Talvey is given in two step-up doses on day 1 and day 4, followed by the first full treatment on day 7. Talvey is given weekly thereafter until disease progression.
- For biweekly (every 2 weeks) dosing: Talvey is given in three step-up doses on day 1, day 4, and day 7, followed by the first full treatment on day 10. Talvey is given every 2 weeks thereafter until disease progression.
- Approximately 1-3 hours before each Talvey step-up dose, you will receive steroids, antihistamines, and acetaminophen. Because of the risk of side effects, you may be hospitalized for 48 hours after administration of each dose in the Talvey step-up dosing schedule.
- Serious side effects of Talvey may include cytokine release syndrome and neurologic toxicities.
- Other side effects of Talvey may include oral toxicities such as dysgeusia (taste disorder), dry mouth, dysphagia (difficulty swallowing), and stomatitis (inflammation of mucous membranes in the mouth); infections, cytopenias (low white blood cell counts and platelet counts), skin toxicities such as skin rashes, and liver toxicity.
- Elrexfio (elranatamab) is the second BCMA-targeted bispecific antibody approved for use as a myeloma treatment. It is given subcutaneously.
- Elrexfio is given in two step-up doses on day 1 and day 4, followed by the first full treatment dose on day 8. Elrexfio is given weekly thereafter through week 24. Responding patients then receive Elrexfio every two weeks until disease progression.
- Approximately 1 hour before each Elrexfio step-up dose and the first treatment dose, you will receive steroids, antihistamines, and acetaminophen. Because of the risk of side effects, you may be hospitalized for 48 hours after administration of the first step-up dose and for 24 hours after the second step-up dose.
- Serious side effects of Elrexfio may include cytokine release syndrome and neurologic toxicities.
- Other side effects of Elrexfio may include infections, cytopenias (low white blood cell counts), and liver toxicity.
- Lynozyfic (linvoseltamab) is the newest approved BCMA-targeted bispecific antibody used for relapsed/refractory patients who have received at least 4 other lines of treatment. It is given as an IV infusion like Kyprolis (carfilzomib).
- Lynozyfic is given in two step-up doses on day 1 and day 8, followed by the first treatment dose on day 15.
- After the first treatment dose, lynozyfic is given once a week through week 11. Afterwards, lynozyfic is given every 2 weeks for 5 doses.
- Based on how well you respond, your healthcare provider will decide if you are able to receive treatment once a month or will continue to have every other week treatment.
- Side effects may include infection, cytokine release syndrome, or neurologic toxicities.
CAR T-cell therapy
Chimeric antigen receptor (CAR) T-cell therapy uses your own white blood cells to fight myeloma. In CAR T-cell therapy, your T cells are collected from your blood, modified in a lab to be more effective in identifying and attacking myeloma cells, and then infused back into your body—as “supercharged” myeloma fighters. These “supercharged” T cells are able to find and kill myeloma cells.
CAR T cells
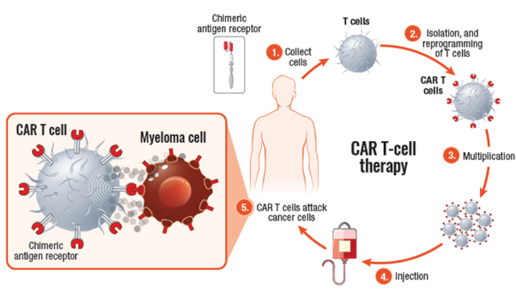
CAR T-cell agents currently approved for use in patients with multiple myeloma include Abecma (idecabtagene vicleucel) and Carvykti (ciltacabtagene autoleucel). Both are BCMA-directed, meaning that the patient’s T cells are collected, altered so that they can recognize BCMA on the surface of myeloma cells, and infused back into the patient, where they kill the myeloma cells.
- Abecma is given intravenously as a one-time infusion 2 days after completing lymphodepleting chemotherapy.
- Carvykti is given intravenously at a one-time infusion 2 to 4 days after you complete lymphodepleting chemotherapy.
- Approximately 30 to 60 minutes prior to CAR T infusion, you will receive acetaminophen and an antihistamine. You will be monitored at least daily for 7 to 10 days following CAR T infusion for signs and symptoms of cytokine release syndrome and neurologic toxicities.
- Abecma and Carvykti are available only through a Risk Evaluation and Mitigation Strategies (REMS) program due to the risk of cytokine release syndrome and neurologic toxicities. Health care facilities that administer CAR T cell therapy must be enrolled and follow the REMS requirements.
-
Abecma is currently approved for patients who are triple class exposed (meaning they have been prescribed and become resistant to a proteosome inhibitor like Velcade, Ninlaro, or Kyprolis, an immunomodulatpry drug like Revlimid or Pomalyst, and an anti-CD38 monoclonal antibody like Darzalex or Sarclisa) and have received at least 2 prior lines of therapy.
-
Carvykti is currently approved for patients who have received at least one prior line of therapy that included a proteasome inhibitor and an immunomodulatory drug, and who are refractory to Revlimid.
Antibody-Drug Conjugates
Antibody-drug conjugates (ADCs) combine a monoclonal antibody with a powerful targeted chemotherapy drug. The antibody specifically recognizes and binds to a protein (antigen) on the surface of cancer cells. After the ADC binds, the cancer-killing drug is released inside the cancer cell.
The FDA has approved one antibody-drug conjugate treatment for multiple myeloma. Blenrep (belantamab mafodotin) is approved for patients who have relapsed after 2 prior lines of treatment.
- Blenrep is a BCMA-targeted antibody-drug conjugate approved for use as a myeloma treatment. It is given intravenously like Kyprolis or Sarclisa.
- Blenrep is administered once every three weeks. Infusion time typically takes 30 minutes.
- Side effects include eye problems, such as blurred vision or dry eyes.
- Other side effects are similar to those seen with many myeloma treatments, like low blood counts and fatigue.
- Side effects are usually managed by dose changes, eye drops, or treatment breaks, and often require close monitoring.
Drugs with novel mechanisms of action
Some of the newest drugs used to treat multiple myeloma do not fit the classification of any existing drugs. These new drugs work in different ways than drugs in the other classes—that is, they have novel mechanisms of action.
Xpovio (selinexor) is the first drug from a category that is referred to as selective inhibitors of nuclear export (SINE). Xpovio is an oral drug typically used in combination with dexamethasone or Velcade and dexamethasone. It is given to patients who have previously received at least four prior treatment regimens and are refractory to proteasome inhibitors, immunomodulatory drugs, and Darzalex.
- Blood tests and body weight are monitored at baseline and during treatment as needed, with more frequent monitoring during the first 3 months of treatment. You should maintain appropriate fluid and caloric intake throughout treatment.
Traditional chemotherapy
Chemotherapy uses drugs that kill cells that are in the process of dividing. Because cancer cells grow and divide more frequently than most healthy cells, they are affected more than normal cells. However, some healthy cells will be affected by chemotherapy, as well. This is what causes side effects. Most side effects can be prevented or reduced.
In the treatment of multiple myeloma, chemotherapy is most often used in preparation for an autologous stem cell transplant, but can also be used if you have relapsed or become refractory to prior treatments and may include these treatments:
- Doxil (liposomal doxorubicin)
- Adriamycin (doxorubicin)
- Alkeran, Evomela (melphalan)
- Cytoxan (cyclophosphamide)
- VP-16 (etoposide)
- Platinol (cisplatin)
- Treanda (bendamustine)
Some chemotherapy drugs are given orally, and some are given intravenously. Often, several drugs are given together, because combining them has been shown to work better at stopping tumors while causing fewer side effects.
Chemotherapy treatments are given in schedules called cycles, which typically last 3 or 4 weeks. Some drugs are taken daily, and others are given weekly or once per cycle. One course of treatment typically consists of four to six cycles, lasting a total of 4 to 6 months.
Steroids
Steroids are another important class of multiple myeloma treatment and are used at all stages of the disease. In high doses, steroids can kill multiple myeloma cells. They can also decrease inflammation, helping relieve pain and pressure. Additionally, steroids may be used to reduce nausea and vomiting caused by chemotherapy and other forms of treatment.
Two steroids that are commonly used in multiple myeloma are dexamethasone and prednisone. They may be used in combination with other multiple myeloma drugs.
Side effects of steroids include high blood sugar, weight gain, sleeping problems, and changes in mood. Over time, steroids may suppress the immune system and weaken bones. These side effects usually go away after patients stop taking these drugs.
Managing Side Effects
Gastrointestinal problems
Many medications for multiple myeloma can cause constipation, diarrhea, nausea, and vomiting. Though some people find it embarrassing to discuss these problems, your doctors and nurses are used to discussing them and can often easily treat them.
Constipation
Your doctor may prescribe a stool softener or laxative to help relieve constipation. Additionally, a diet high in fiber with plenty of fruits, vegetables, lentils, whole grains, and bran-based cereals can help. Drinking plenty of water is important, and hot drinks like coffee or tea can help stimulate a bowel movement. Gentle exercise, such as walking or swimming, can also be helpful.
Diarrhea
If you experience severe diarrhea (more than six loose stools per day for two days), let your doctor know right away. He or she will recommend an antidiarrheal medicine (either over-the-counter or prescription) and may advise you to take a fiber supplement. It’s important to stay hydrated when experiencing diarrhea, so drink plenty of water and avoid coffee and alcohol. Eating small, light meals slowly throughout the day can be helpful.
Nausea and vomiting
Nausea is commonly experienced by people with multiple myeloma, due to the disease itself or to certain treatments. Drugs called antiemetics are used to treat nausea and vomiting. Depending on the multiple myeloma treatment you’re receiving, your doctor may even prescribe an antiemetic drug to stop nausea and vomiting before it starts. Drinking lots of fluids and eating small meals throughout the day can also help manage nausea and vomiting.
Decreased blood counts
Decreases in blood cell count can be caused by multiple myeloma itself and also by many myeloma therapies. Proteasome inhibitors such as Velcade and Kyprolis, immunomodulatory drugs such as Revlimid and Pomalyst, and antibodies such as Empliciti can decrease the numbers of red blood cells, white blood cells, and platelets.
Blood cell counts are carefully monitored by your doctor. If they become too low, myeloma therapy may be delayed or dose adjustments may be made until the blood cells increase to normal levels.
Maintaining good nutrition is important in helping blood counts stay in the normal range. Your doctor may also prescribe growth factors such as erythropoietin to stimulate red blood cell production and/or colony-stimulating factors such as G-CSF or GM-CSF to stimulate white blood cell production.
Infection
Though multiple myeloma patients are at higher risk of infection because of the disease itself, many myeloma treatments also increase the risk of infection because of their effects on blood counts—specifically white blood cells, which help fight infection.
Cytokine release syndrome
Cytokine release syndrome (CRS) is a common and serious side effect of bispecific antibody and CAR T-cell therapies. CRS can occur after infusion of the therapy. It causes fevers, chills, and low blood pressure. For this reason, your healthcare team will closely monitor you after treatment for signs of CRS. Treatment for CRS may vary but will generally include medication to reduce inflammation, as well as other treatments depending on your symptoms.
Neurotoxicity
Neurotoxicity is another serious complication that may result from bispecific antibodies or CAR T-cell therapy. Most patients experience mild symptoms like confusion but, in some cases, patients experience severe symptoms like delirium or seizures. Your healthcare team will take steps to minimize the likelihood of neurotoxicity, monitor for symptoms, and promptly treat it.
Supportive Care
Explore complementary care, adjunctive treatments, and, when needed, hospice options. Be sure to speak with your healthcare team if you feel you would benefit from any of these supportive care approaches. Some medical centers may offer such services for free or at a reduced cost for cancer patients.
Radiation therapy
Radiation therapy, which uses high-energy particles or rays to damage cancer cells and prevent them from growing, has proven effective in treating complications from bone disease caused by myeloma. In low doses, local radiation therapy (radiation delivered to a specific part of the body) can help relieve uncontrolled pain or prevent or treat bone fractures or spinal-cord compression. In high doses, local radiation therapy (sometimes given with chemotherapy) is used to treat solitary tumors in bone or soft tissue (plasmacytomas). Radiation therapy may also be called radiotherapy, x-ray therapy, or irradiation.
Adjunctive treatments
In addition to receiving medical treatments directed at managing your disease, you will most likely require additional treatments to help manage symptoms and treatment side effects.
Drug therapies can help relieve multiple myeloma symptoms, such as bone disease or kidney failure and side effects from treatments such as blood clots.