
How did you get involved with the MMRF?
Team Papa JJ was formed nearly two years ago for the 2022 MMRF Walk/Run: Washington, DC. Douglas J.J. Peters, affectionately known as “Papa JJ” by his grandchildren, was a few months into his multiple myeloma diagnosis.

Why did you choose to participate in the MMRF Walk/Run?
Doug’s diagnosis forced him to step away from work and receive fatiguing treatments at home. He loved working with people and took pride in his fitness, so his newfound isolation and weakness proved to be an adjustment. When he became aware of the MMRF Walk/Run in the county he called home, he jumped at the chance to join.
He took to social media to make his multiple myeloma battle public while inviting others to join in, posting “My diagnosis and path to remission inspire me to do what I can to help others fight this cancer and to further accelerate efforts toward better treatments and a cure for multiple myeloma.”
The event offered the opportunity to set a fitness goal, walking a 5k route under his own power after months of bed rest; connect with friends, family, colleagues, and loved ones he had not been able to see; and most importantly, join other patients to HELP FIGHT multiple myeloma TOGETHER!
Together at the 2022 and 2023 MMRF walks, Team Papa JJ raised over $45,000 and rallied over 175 walkers!
The MMRF walks gave Doug great joy, pride, and most of all, hope. He bonded with other patients who had been living with multiple myeloma for years or even decades. They eagerly showered him with encouragement and inspiration.
Unfortunately, Doug passed due to complications from his treatments a few days after Christmas this past year. He was surrounded by his family and loved ones.

The Spirit of Hope is given to “individuals/groups who inspire hope and show extraordinary commitment to the MMRF.” What does being given the award mean to you?
Team Papa JJ is honored to receive the Spirit of Hope award. Participating in the MMRF walk was Doug’s idea, and meeting other patients leading fulfilling lives while fighting myeloma gave him great hope. His choice to actively fight against the cancer with others instead of bemoaning his situation inspired donors and walkers alike to join the fight. We see the award as a public acknowledgment of the inspiring fight we saw in private, and we are grateful for the recognition. We hope teams and participants in this year’s Walk/Run are able to take advantage of the event’s unique opportunity to bring people together in the name of optimism, hope, and love to continue the fight against multiple myeloma.
How have you found perseverance in light of obstacles? Please share any stories that have given you strength.
Doug was a strong, competitive man by nature who thrived on challenge and helping people. Whatever he chose to do, he was going to give 110%! It was wonderful to see Doug combine his fighting spirit with his strong fundraising capability to fund the fight and find a cure. The endeavor gave him joy and purpose.
Doug knew he could only do so much to control the cancer, so he set out to control each day. When his body was at its weakest, his mind was at its strongest, and he remained driven. He learned to set smaller, more manageable goals he could complete each day. These included knocking five things off his “to do” list daily and beginning each day reading scripture during his 20-minute Peloton ride. Doug persevered through faith and bountiful HOPE, exhibiting humility, grit and grace throughout his battle. He vowed never to let multiple myeloma break his spirit. With hope, he fought to the end.

Does your team have a favorite mantra, quote, lyric that gives you strength?
Doug was a man of faith and an avid movie fan, making it fitting to include his favorite Bible verses alongside a quote from his favorite film.
“What good is it, my brothers and sisters, if someone claims to have faith but has no deeds? Can such faith save them? Suppose a brother or a sister is without clothes and daily food. If one of you says to them, “Go in peace; keep warm and well fed,” but does nothing about their physical needs, what good is it? In the same way, faith by itself, if it is not accompanied by action, is dead” (James 2:14–17).
“What we do in life, echoes in eternity” (Maximus Decimus Meridius, Gladiator)
The Team Papa JJ In honor of Douglas J.J. Peters, MMRF 2024 Walk/Run: Washington, D.C. Spirit of Hope Honoree. Donate to Team Papa JJ as they accelerate a cure in Douglas’ memory.
This award is presented at every Walk/Run to a patient, caregiver, or family who inspires hope through their resilience, perseverance, and dedication to the MMRF and its mission.

I was diagnosed with MGUS in June, 1993, but my primary care physician and my first three oncologists all led me to believe that I already had active multiple myeloma. Since I am a retired scientist, I began a continuing quest to educate myself about all things myeloma. That was greatly helped when I joined the North Texas Myeloma Support Group (NTMSG) in April 2004. This support group meets in Dallas monthly with patient sharing and guest speakers. In a very real sense, those support group members became a part of my extended family, and many are now good friends. I am now a technical resource to help find answers to questions from other support group members. My wife and I do not have any children. Our immediate and extended families all live at least 900 miles away. So, my Dallas support group is a significant part of my social family.
I became involved with the MMRF after discovering that they are a very good reputable resource for myeloma education. The more I learned, the more I was impressed with how professionally run, organized, and effective the MMRF seemed to be. I was especially impressed with the creation of the Multiple Myeloma Research Consortium (MMRC). The MMRC used critical business processes to accelerate the rapid initiation and completion of Phase 1 and 2 myeloma clinical trials by eliminating much of the prior competition to complete and publish research results individually. Each organization member specializes in what they do best and then shares the credit and quicker publication of results.
I was also very impressed with the MMRF CoMMpass study. It focused on mapping the genomic landscape of myeloma to understand patient subtypes and risk stratification and identify new targets. These results are available in the public domain for all myeloma researchers. It was the first study to identify twelve subtypes for myeloma related back to DNA alterations. This identified actionable DNA alterations for personalized treatment that became available in the MMRF MyDRUG clinical trial.
I was also impressed with the goals of the MMRF CureCloud study. This was one of the largest longitudinal data sets to collect myeloma patient information to help direct future myeloma research efforts. I participated in this CureCloud project.
I am a retired scientist formerly employed by a Johnson & Johnson company that manufactured hospital laboratory testing materials and human injectable products (derived from human blood). Therefore, I know the importance of clinical trial participation to get new myeloma treatments evaluated and FDA approved. For this reason, I have already participated in three clinical trials to do my part to help this process.
I feel that the MMRF does a particularly good job of efficiently using donated funds to produce very significant myeloma research knowledge results that are then put to practical use. A NTMSG member and friend, Patrick Beal, began organizing and captaining a team for the yearly MMRF Dallas Walk/Run fundraisers. I have always joined that MMRF fundraising team to support Patrick and that effort. For that reason, I consider this Spirit of Hope award to be a team effort. I give the credit to our North Texas Myeloma Support Group (NTMSG) MMRF 5K Walk/Run yearly fundraising teams. We tend to come in second or third most years in our fundraising success against much larger teams and organizations. This Spirit of Hope award acknowledges our team accomplishments in fundraising for such a worthwhile cause.

My personal philosophy for managing my myeloma mandates having hope, sharing the hope, and continuing education. Whatever happens, happens for a reason. Always remain positive about your life.
I take a lot of inspiration from Jim Valvano’s 3/4/1993 ESPY speech: “Cancer can take away all of my physical abilities. It cannot touch my mind, it cannot touch my heart, and it cannot touch my soul.” Valvano was an American basketball player, coach, and broadcaster. The motto for the Jimmy V Foundation for cancer research is “Don’t give up! Don’t ever give up!”
The MMRF is delighted to recognize Dennis McClure as the MMRF 2024 Walk/Run: Dallas Spirit of Hope Honoree. We encourage you to donate to his team the North Texas Myeloma Support Group (NTMSG)
This award is presented at every Walk/Run to a patient, caregiver, or family who inspires hope through their resilience, perseverance, and dedication to the MMRF and its mission.

How did your team get involved with the MMRF?
My brother Ophire was 35 years old when he was diagnosed with multiple myeloma in September 2008. He was in contact with Kathy Giusti and found out about the 2016 MMRF Walk/Run 5K in Boca Raton. He fought long and hard for eleven years, flying back and forth to NY for treatment. He endured endless rounds of chemo, radiation, three stem cell transplants, six clinical trials, eight different drugs, and emergency spinal cord compression surgery.

Why did your team choose to participate in the MMRF Walk/Run?
Ophire decided to become a “patient activist” to help advance the development of new drugs brought to market. He created No Fear Warrior to inspire hope and demonstrate the resilience of those who are alive and fighting MM. A large group of friends and family came out year after year to run and walk alongside him while he fought for his life. Ophire passed away surrounded by the love from his family and friends in January 2020 at 46 years old. Ophire didn’t die from myeloma; he died battling against myeloma. No Fear Warrior has continued to fundraise to keep his memory alive.

The Spirit of Hope is given to “individuals/groups who inspire hope and show extraordinary commitment to the MMRF.” What does being given the award mean to you and your team?
It is an honor for Ophire/No Fear Warrior to be recognized with this award. Receiving this award means that while Ophire is not with us, his spirit and memory lives on. We hope to carry the torch of inspiration and will continue to fight for a cure in our lifetime!
How has your team found perseverance in light of obstacles? Please share any stories that have given you strength.
God gives his toughest battles to his strongest warriors. Ophire was the most courageous, brave, man that I knew – he was a warrior that never gave up. He was an inspiration and touched so many lives with his positive attitude and zest for life. He had a 1000-watt smile that could light up a room. He was a respected leader in his profession and also had the ability to be your friend, which is very hard to do. In all my life, I’ve never heard anyone speak badly about Ophire. Everyone who knew him loved him.

Does your team have a favorite mantra, quote, lyric that gives you strength?
Ophire’s signature in his email was initially “Attitude is a little thing that makes a big difference” and later “Life is good.” His Facebook cover had the quote “Never, never, never give up” by Winston Churchill.
Anything to Add?
We’re looking forward to meeting our family in Tampa this November to walk in Ophire’s memory and support the MMRF!
The MMRF is delighted to recognize Team No Fear Warrior In honor of Ophire Jericho as the MMRF Spirit of Hope Honoree at the 2024 MMRF Team for Cures: Tampa Walk/Run. Donate to their team today to accelerate a cure!
This award is presented at every Walk/Run to a patient, caregiver, or family who inspires hope through their resilience, perseverance, and dedication to the MMRF and its mission.

How did your team get involved with the MMRF?
I was diagnosed in July 2022 with multiple myeloma, and it was a shock to everyone. I had been having some back pain that was worsening, and I finally ended up in the emergency room. That evening in the ER after hearing this diagnosis, I was admitted and began the fight for my life. After surgery, radiation and starting chemo, I was discharged in August 2022, and I came across MMRF in the pile of resources given to me. I went online to check out their work and immediately wanted to be a part of their activities. Our family and friends signed up for the walk, and our team, the Myelominators, was able to raise over $7,000. We wanted our name to be somewhat lighthearted but reflect our commitment that myeloma cells, or Myelomans as we were calling them, must DIE! It was a bite off of The Terminator movie, which involved a lot of killing—in our case, we wanted all myeloma cells to be annihilated!

Why did your team choose to participate in the MMRF Walk/Run?
This is somewhat addressed in the question above, but team members wanted to show support for me and our family after hearing about my diagnosis. We had colleagues, friends, and family join us to show that I wasn’t alone—that they cared about my family and were sending their positive thoughts to me as I was fighting this cancer. Team members also wanted to raise money for this important cause, not just for me, but for all the families affected by MM. The new treatments mean life or death for so many patients, and anything we can do to advance this cause must be done.

The Spirit of Hope is given to “individuals/groups who inspire hope and show extraordinary commitment to the MMRF.” What does being given the award mean to you and your team?
On a personal level, this award has given me a tremendous psychological boost. Five months after diagnosis, I received a stem cell transplant in December 2022, and it seemed to be a success. I finally had the headspace to further educate myself about this disease. During this time, I watched MMRF webinars and read articles. Despite being in remission (or so I thought!), I wanted to continue to support MMRF in their efforts to fund myeloma research. I read so much about the advances in long-term outcomes and improved quality of life for MM patients due to the advances in medications, treatments, and so forth, all of which came from research activities that MMRF funds. Therefore, I gathered friends and family again for the 2023 MMRF Walk. In addition, my husband (and team member), Vik, had decided to set a goal of participating in Moving Mountains for Multiple Myeloma in 2025. Moving Mountains required a higher financial commitment, and we were ready to take that next step to an organization that was dear to our hearts.
Coincidentally, I first heard of Dr Amrita Krishnan’s name from a MMRF patient webinar in the summer of 2023. She is a world-renowned expert on relapsed/refractory MM at City of Hope. As fate would have it, I relapsed in November 2023, and after treatment from December to February 2024, I was referred to Dr. Krishnan for treatment options. Dr. Krishnan recommended CAR-T therapy, and I’m scheduled for this treatment in May 2024. I can firmly say that through their fundraising activities and patient education resources, MMRF has played a meaningful role in guiding my MM journey, especially during this new phase of relapse. I tell all my friends, CAR-T with Carvykti wasn’t even an option in 2022 when I was diagnosed—it was only through research, clinical trials, advocacy with organizations such as MMRF and researchers such as Dr Krishnan that this advance was pushed through and is now available to patients like myself.

How has your team found perseverance in light of obstacles? Please share any stories that have given you strength.
Persevering is a true challenge. It takes active thought and energy. After discovering my relapse in December 2023, we were all devastated. We were just barely recovering from my diagnosis the year prior. I hadn’t even been in remission for a year. This time, the physical limitations and pain experienced were very significant. The feeling of being overwhelmed was greater than ever because we were monitoring my cancer with labs, and it had quietly converted to a non-secretory form of melanoma, so we had no idea it was back until all the physical symptoms had manifested.
We took strength in our family, friends, and supporters who kept pouring in. Even people we didn’t know or have a relationship with were offering to help. The sense of humanity, compassion, and empathy of so many around us—that brought us tremendous strength. It kept us going day after day.
For me, I meditated on the workings of the universal consciousness. I remember the words of Abraham Lincoln: “The best way to predict the future, is to create it.” As a family, we were determined—I would not be a “statistic.” I was creating my outcome. In fact, from a quantum consciousness perspective, I was already healed and cancer free. Embedding these ideologies in my mind, I took one step at a time, one day at a time. This journey is actually filled with love, laughter, joy, and immense pain. Yet, I will persevere. I’m just going through the process—biding time until final success is achieved and I am myeloma free.
From my sister-in-law, Divya, “You are always authentic and real. The strength you’ve demonstrated in these past two years gives me confidence that I can also approach difficult situations with confidence. You are a symbol of toughness beyond many men and women.”
From my brother- and sister-in-law, “Archana has been a tremendous inspiration to us for her unwavering positive attitude through this. She’s a fighter and a winner, and it’s been a privilege to see her triumphs. Keep up the fight; we’re in your corner. Always!”
From a friend (J.R.R. Tolkien), “It’s not the strength of the body that counts, but the strength of the spirit.”
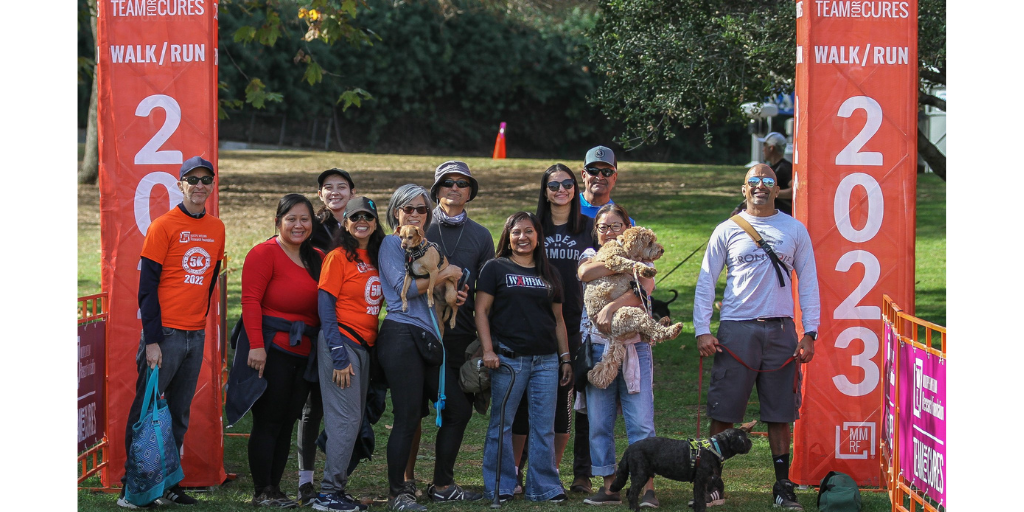
Does your team have a favorite mantra, quote, lyric that gives you strength?
Fight to Win! FTW!
The MMRF is delighted to recognize Archana More Sharma as the MMRF Spirit of Hope Honoree at the 2024 MMRF Team for Cures: Los Angeles Walk/Run. Donate to “The Myelominators” today to accelerate a cure!
This award is presented at every Walk/Run to a patient, caregiver, or family who inspires hope through their resilience, perseverance, and dedication to the MMRF and its mission.

I’m extremely flattered by being the individual chosen to receive this year’s MMRF Spirit of Hope Award for the Twin Cities 5K Walk/Run fundraising event. But unfortunately, it’s also partly the result of being a multiple myeloma patient, which means I have a cancer that currently does not have a cure. And that is by far the number one reason I’m passionate about doing my part to help find a cure for this disease. But it’s not just about me—it’s about all the other myeloma patients and caregivers I read about, listen to through Patient Webinars, and see at Lake Phalen every year doing everything they can to help find a cure for us patients, so we and future myeloma patients can live a full life with all those individuals who love us so much.
A few other organizations are out there that are also working to find a cure for myeloma. So that begs the question: Why did I choose the MMRF as the organization I wanted to put my time and energy behind? To determine that, I asked myself a pretty simple question: What is the best possible way to find a cure for myeloma? I believe the answer is through research. When I looked at the track record of the various organizations, two stood out to me because of the number of years they’ve been in existence, and they both were started by individuals who were directly impacted by myeloma. Two criteria separate the MMRF from all the others: over 90% of the funds it raises go directly toward research, and it has a major fundraising event right in my backyard. Bingo! We have a winner! Just look at the amount of money the MMRF has given to date toward research, over $600 million! Yes, over $600 million dedicated directly to finding a cure for myeloma. All of us need to do our part in helping to generate more funding for research, so we have a chance to win our fight to live and realize the love of all our family members and friends who have been there for us because they want us to live.
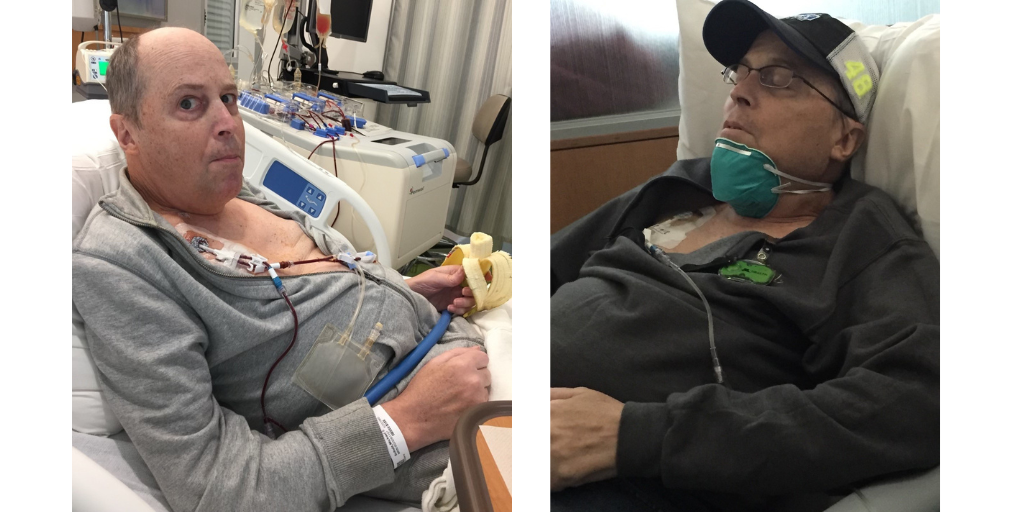
What I admire the most are those family members and friends that have continued to help raise money for research, in spite of the fact that their loved ones that they fought for fell short of winning their battles. These are the ones who most emulate what the Spirit of Hope stands for, and they are the true winners of this award. Last year four teams raised over $10,000 for the 5K Walk/Run fundraising event, and my team was one of them. But get this, the other three teams raised their donations in remembrance of loved ones who used to stand with us Living Proof members in years gone by now, and those teams continue to act because of what those people meant to them, and don’t want our caregivers to have the same results as they did.

HOPE. It’s a word that carries a heavy load. It’s also a word that I believe in. I do have hope. When I was first diagnosed back on January 17, 2012, I was told I would be lucky to live a year and a half. I’ve relapsed two times and have participated in two clinical trials. Twelve and a half years later, I’m still here. Why? I have a lot of faith and believe that God wants me to still be here for a reason that only He knows. In addition, since I was first diagnosed, eleven new forms of treatment have been approved by the FDA, I’m currently on one of them (daratumumab or Darzalex) for maintenance. A whole new field of treatments is coming on the scene and is starting to explode with different variations. I’m talking about immunotherapy, which includes CAR-T therapy and bi-specific therapies. The results are extremely promising. And that means HOPE—hope that someday soon, we’ll yes, we’ll find a cure. Join me and my team, The Mike Schulz Marchers, at this year’s Twin Cities 5K Walk/Run Fundraising event. Let’s give the Living Proof photo a whole new meaning.
Sincerely,
Mike Schulz
The MMRF is delighted to recognize Mike Schulz as the MMRF Spirit of Hope Honoree at the 2024 MMRF Team for Cures: Twin Cities Walk/Run. Donate to his fundraising page to accelerate a cure today!
This award is presented at every Walk/Run to a patient, caregiver, or family who inspires hope through their resilience, perseverance, and dedication to the MMRF and its mission.

Joe McMahon, founder of First Knight Racing and host of the Peasantman Steel Distance Triathlon, has dedicated himself to organizing, directing, and participating in races since the age of 20.

With an impressive athletic resume boasting over 500 races, including 38 full distance triathlons (four of them Steel Distances), 75+ marathons, and 17+ half distance triathlons, among others, Joe has earned widespread respect within statewide triathlon clubs and unofficially holds the #2 spot for most full distance triathlons completed in New York State.
Passionate about making a difference, Joe has contributed significantly to charitable causes, raising over $920,000 for various charities, including the MMRF.

Reflecting on his passion for fundraising and its personal significance, Joe shared: “Fundraising for important causes has always been at the forefront of my racing career. In 2013, I met the inspirational team at MMRF, and was immediately drawn to their mission to further pharmaceutical research and improve patient outcomes. My father, Dr. William McMahon, was diagnosed with multiple myeloma, so the cause is near and dear to my heart.”
In early 2024, Joe reconnected with former MMRF Ironman Lake Placid teammate, Salim Martin, who currently serves as the MMRF Endurance Coach. Their discussions led to a new partnership between First Knight Racing and MMRF for the 2024 Peasantman Steel Distance Triathlon.
With unwavering commitment to advancing the MMRF’s life-saving mission: to accelerate a cure for each and every patient, Joe stated: “Every penny raised through this partnership will go directly to MMRF. The First Knight Racing organization couldn’t be prouder to begin raising money to support this critically important cause, and we are eternally grateful to MMRF for their collaboration.”
Secure your spot and make history by joining MMRF Team for Cures at our inaugural participation at the Peasantman Steel Distance Triathlon.

Eric Gelber, a CBRE Executive Vice President and ultra-endurance athlete, a husband and father has taken on increasingly challenging endurance feats to raise funds to find new treatments and eventually a cure for multiple myeloma, a blood cancer which, currently is incurable. Eric has raised over $2,400,000 for the Multiple Myeloma Research Foundation (MMRF) to fund critical research to accelerate a cure for every patient.
It began in 2006, when Eric decided to get off the couch and run his first marathon to raise funds for cancer research and honor a friend, Anita, who was battling multiple myeloma. After that first marathon he was hooked. Each year since then, he has challenged himself by taking on longer and more difficult events, building up to The Journey Towards a Cure in 2016. On his third attempt, over the course of 60 hours, Eric ran 200 Miles in New York City’s Central Park. Hundreds of everyday runners, patients and caregivers joined him as he put his body on the line to raise money and awareness for the MMRF. Eric’s incredible story has attracted much media attention. In 2016, Resonant Films and Tribeca Films captured his passion and grit in a 50-minute documentary, 200 MILES, which premiered at the prestigious TriBeCa Film Festival and is now available on Crackle and a number of other streaming services.
In 2018, Eric reimagined The Journey into a festival like atmosphere which included a 12-hour run relay, live music, and a food and beer garden. Most importantly it was a chance for all to come out to support and celebrate life together at a one-of-a-kind event. The event inspired nearly 150 people to push their limits to support myeloma patients, raising over $194,000. Then In 2021, he returned to Central Park but not for a run, but another epic idea created by Eric, a 200-mile erg rowing event! The rowing event raised $165,000 pushing the total raised by Eric and supporters of The Journey to over $2 million to accelerate a cure.
On April 27-28, 2024, Eric invites you to be part of The Journey at Sea Colony a family-friendly 2-day event that will encompass an exclusive viewing of the inspiring 200 MILES documentary and cocktail party, tennis and pickle ball tournaments, and a 5K race and 1-mile fun walk. Register now for the event or make a donation to The Journey today!
My big moment with the MMRF came on February 20, 2018, about a year after being diagnosed with multiple myeloma. I had gone through ~12 months of testing, treatments, and a successful stem cell transplant, and as most myeloma patients will tell you, that first year was very structured. The path to remission seemed very well known, and there were expert oncologists and nurses there to help define a daily routine for me, which gave me great comfort.
But then came 2018, when it was time to transition to maintenance therapies and settle into a less-structured “normal life” living with cancer. There was just one problem: living with cancer wasn’t normal for me! I remember feeling very intimidated about taking that step. What if I don’t know how to live with cancer? What if I do it wrong? What if I make a mistake!? What if it all comes crashing down?!?!
My wife Katie, being the emotionally intelligent one, recognized that really, I just needed to talk to someone about my feelings, and she guided me to the MMRF. I agreed to reach out because deep down I just wanted to find someone else like me—someone who had dealt with these feelings before—someone who was out there living a normal life with cancer. That’s when I got my first email from the MMRF.
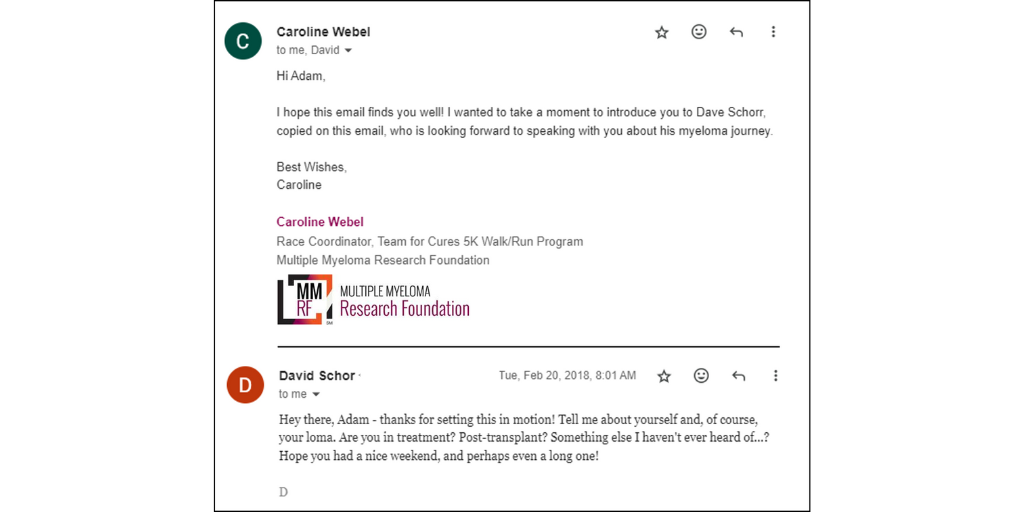
Caroline Webel from the MMRF in Norwalk, CT, understood what I was feeling, and she introduced me to a gentleman named David Schor. Dave was a myeloma survivor from New Jersey who (for some odd reason) liked the Denver Broncos. He was living proof that you could be a cancer patient and a dedicated sports fan and a Dad and a husband and a regular dude all at the same time. He loved his wife and his son and his beagle and especially Boston accents. He enjoyed his job and fitness and taking risks and watching funny movies and all the same things that I wanted to have in my “normal” life with cancer. And he did it all with such a carefree attitude too. I will never forget the first email I got from Dave. He didn’t call our disease by its real name, he simply referred to it as “Loma”. Ha ha, he had a nickname for it! It was clear that he had accepted cancer, like it was just another part of him, like anything else would be. Cancer did not define him, and that gave me hope.
Now many years later, Dave and I are still close friends, each living our best cancer lives thanks to the MMRF. Our friendship is largely a remote and virtual one—held firmly together by sending text messages and Christmas cards, comparing test results, and sharing medical data and links to emerging myeloma treatments. Most importantly though, we share the laughter of a 100 million inside jokes that have come to life since the day Caroline Webel introduced me to my “Chemosabe”:

The credit for discovering the MMRF Walk/Run and choosing to participate belongs entirely to my lovely wife Katie. Since forming our first MMRF team in 2018, she has accumulated over $75,000 in donations for the Boston event and inspired hundreds of generous runner-walker-donors to get involved and join us along the way.
Included on the annual team are our two young children, Cali and Tyler, who have also been active fundraisers and participants since our first MMRF Walk/Run. Incidentally, that brings up another brave decision that I credit to Katie: the choice to inform and educate our kids about what it means for Dad to have cancer. The truth hurts sometimes, but we never hid it from them. Katie helped me be up front and honest about my diagnosis with Cali and Tyler, which brought understanding for them and eventually healing for us all. Now they share in the excitement of preparing and participating in the MMRF Walk/Run every year.
Through the MMRF Walk/Run, Katie has created a tremendous amount of momentum with many other “True Believers” out there who will not back down and insist on winning the fight against myeloma. Here are just a few photos of the team.

In my personal battle with myeloma, I have always been able to draw strength from music. Very specifically, I am motivated by punk rock bands from the 1980s and 1990s who, after grueling 30-year and sometimes 40-year music careers, still manage to get up and go out and sing their punk rock anthems year after year. I admire these groups for standing up for what they believe in for so long. I also imagine it takes great physical strength to endure decades of songwriting, record making, and concert touring to promote their musical message.
It gives me hope to know that these musicians are able to persevere, even as their bodies age. Their songs have survived for all these years, and knowing that helps me overcome obstacles on my own long-term journey with myeloma.
Do you have a favorite mantra, quote, lyric that gives you strength?
As a matter of fact, I have many! Here are a few recent photos of the durable musicians discussed above and an example of a song lyric from each. These lyrics give me hope and strength every day. (Note, these are all personal photos I took in the last year, proof that the music and this patient are both still strong today!)



It means that it’s working—the medicine, the fundraising, the research, those ugly days and hospital nights and long drives and hot/cold/rainy/windy laps at the MMRF Walk/Run. It means it’s all working. As cancer patients, we all need that validation every once in a while: a reminder that not only is there a light at the end of the tunnel, but’s it’s getting brighter and brighter all the time.
I am thrilled to share this Spirit of Hope recognition with all the friends, family, patients, MMRF reps, walk/run volunteers, punk rock bands, Chemosabes, and True Believers out there. Thank you from the bottom of my heart for the hope and validation you provide us every single day!
The MMRF is delighted to recognize Adam Ralston as the MMRF Spirit of Hope Honoree at the 2024 MMRF Team for Cures: Boston Walk/Run. Donate to his team “True Believers” to accelerate a cure!
This award is presented at every Walk/Run to a patient, caregiver, or family who inspires hope through their resilience, perseverance, and dedication to the MMRF and its mission.
I want to share an inspirational story about one of the athletes I train. His name is Marc Schiff (@maschiff), he’ll be 61 years “young” next month, and I’ve been working with him since 2017. While Marc has been athletic his entire life, he never considered himself a runner. And although he ran track as a sprinter for a couple of years in high school, running was more of a necessary evil to stay in shape for baseball and lacrosse. Then, in late 2012 a cancer survivor friend asked him if he’d run a 5K in Phoenix to benefit Colon Cancer. He thought what the heck, why not, it’s only 3.1 miles! So he worked his way up to the distance on a treadmill over a few weeks leading to race day and was ready to go. Little did he know his life would be changed forever! He ran a 28:43 5K which was good for a 6th place AG finish. One year later he ran the same 5K in 23:51 and landed on the podium, and all of sudden he became a runner! Since then Marc has completed 25 half marathons, 2 Ragnar Road Relays, 3 full marathons and countless 5Ks, 10Ks and 15Ks. He’s also run Pat’s Run 7 years in a row and the Mesa-Phoenix Half/Full 6 straight years.
I met Marc for the first time in 2016 at the Gilbert Half Marathon Expo and started working with him shortly thereafter. He felt like he was stagnating at the Half Marathon distance and wanted to work his way up to the Full. His first Full Marathon was the 2017 Rock ‘n Roll Arizona and he finished at a respectable 4:27. But he wasn’t the least bit satisfied. He went back to work and set his sights on the 2017 Rock ‘n’ Roll San Diego full. Unfortunately, he tore a hamstring 10 days before the race during his last long run and it was back to the drawing board. Marc worked his way back and his next goal race was the 2018 Mesa-Phoenix full. We set his A Goal at 4:15 which would be a stretch but not completely out of reach. He ended up finishing in 4:18 with an unplanned porta-potty stop at mile 21! That was good for a 9 min PR! Still not satisfied, Marc’s next goal race was the 2018 NYC Marathon. This was particularly special for him as he and his entire family are from Brooklyn and he hadn’t been back in almost 40 years. Marc’s training was going well, and he wanted to set his sights on a 4:00 finish. Knowing the course well I told him that was too aggressive so we backed it down to 4:15. Then, once again, injury struck, this time a stress fracture in his left foot! After 8 weeks in a boot NYC was out of the question so he had to defer to 2019. Once again it was back to work, this time essentially starting over. I eased Marc back to running slowly and by June he was pretty much back to his pre-injury fitness level, running the Rock ‘n’ Roll Seattle Half in 1:57. He was healthy heading into NYC with his final long-run being a 2:01 finish at the Lake Powell Half in October. Because of his previous injuries we decided not to set a goal time for NYC and instead just run for the experience of it all and have fun. He finished in 4:33, which for that course, and considering the huge crowds and multiple bridges, isn’t anything to be ashamed of.
Now most runners would be satisfied to take a break for a few months, but not Marc. He was already registered for the Rock ‘n’ Roll Arizona Half in January and Mesa-Phoenix Full in February! Thankfully I was able to talk some sense into him and he dropped down to the Half for Mesa-Phoenix, which by the way, he ran in 1:58! Little did we know this would be the last live race before COVID-19 shut everything down. I’m sure it’s no surprise that he embraced the virtual racing phenomena head first. Not only did he run virtual races almost every weekend, but he organized and led a weekly Virtual Group Run that attracted more than 50 runners from all over the US as well as Canada, New Zealand, Australia and England! This week will be the 8th.
So now that I’ve given you a sense of Marc’s grit and determination, this next part is where the real inspiration comes in. On May 7th, I got a text from him telling me that he had just been diagnosed with Multiple Myeloma, a relatively rare form of blood cancer. This particular cancer is in the bone marrow and it primarily affects the white blood cells that defend the body from infection and fight viruses. Instead, the cancerous white blood cells crowd out the healthy cells which results in a compromised immune system; not good ever but especially during a global pandemic! And if that’s not bad enough, the cancerous cells attack the bones from the inside out and cause “cystic lesions”, which in layman’s terms are holes in the bones. A PET Scan showed “innumerable” lesions throughout his body. This condition causes localized bone weakness and makes him much more prone to stress fractures, a runner’s nightmare. Marc started chemotherapy a week later and has just completed his first cycle. While the first results look promising, this is the “marathon of all marathons”. One without a finish line. There is currently no cure for Multiple Myeloma, although it is treatable. And luckily for Marc, it was caught in Stage 1. But the road ahead will be long and hard. Weekly chemotherapy treatments for 6 months followed by a Stem Cell Transplant to essentially wipe out the bone marrow and start over. He’ll then be on maintenance medication for the rest of his life. The side effects of the chemo are not fun; nausea, fatigue, insomnia, neuropathy and weight gain from taking highdose steroids. Add a compromised immune system on top and you get the picture.
I spoke with Marc yesterday and he said he’s doing pretty well under the circumstances. He sounded upbeat and positive. I was expecting him to say he wanted to discontinue coaching, but not surprised at all when he said just the opposite! He told me that he wanted to keep running as long as his body allowed it. He wants the accountability of having a plan to follow. He wants to remain a part of the BTB team and stay connected to the running community. He’s willing to roll out of bed at 5:00 am to beat the Arizona heat. I actually saw on Strava that he ran a 10K this morning at 6:00 am! And for those days that he can’t, he’s purchased a treadmill so he can run later in the day. If that’s not dedication, I don’t know what is. When we talked about me sharing his story on Instagram he made a point of telling me that he doesn’t want people’s pity or to be treated special because of his condition. He’s a runner who happens to have cancer, not a cancer patient who happens to run. He wants to bring awareness to this cruel disease and provide hope and inspiration to those who are also facing hardships and adversity. A positive outlook and strong network of supporters can work miracles.
If you’d like to learn more about Multiple Myeloma, or make a donation to help fund research to find a cure and make treatment more affordable, Marc’s posted some links in his profile. You can follow him to keep up with his journey. While there may be no new PRs for the foreseeable future, this is a race that he must win, and I’m 100% confident if anyone can it’s Marc

My involvement with MMRF started in 2019 while I was undergoing my induction therapy. I was at my infusion center for one of my weekly treatments and decided I wanted to do something to help find a cure for Multiple Myeloma. I came up with an idea to create a t-shirt that I could sell to raise money that would be donated to the MMRF. I’m an avid runner and part of a huge Facebook group of runners who I knew would be more than happy to purchase one. I sold the shirts at cost and asked people to add whatever donation they could. I ended up selling 80 shirts and raised $1800. With my company match, $3,600 was donated to the MMRF.

I chose the MMRF Walk/Run for several reasons, the most important being that I am a multiple myeloma “survivor” myself. I was diagnosed in April 2019 and underwent a stem cell transplant in November 2020. Knowing that there is no current cure, I want to make whatever difference I can, and participating in the MMRF Walk/Run is one way to do so. I also enlisted fellow runners, friends, and family to participate in person or virtually or to just donate.
I am so humbled to receive this award. Since my diagnosis, I have tried my best to be a role model for other myeloma patients or anyone dealing with similar life-altering diagnoses. I used social media to document my journey to inspire others and instill hope. I continued to run during my induction therapy and made a commitment to myself to run a half marathon within 6 months of my stem cell transplant. I even registered for one a day after my transplant! I lived up to this commitment by running the Glacier Half Marathon in Montana in May 2021. I wanted to show others that you don’t have to be defined by the disease.

As I’ve mentioned several times already, I’m an avid runner and have a wonderful community that supports me. One special running friend, Julie Love, who was the same age as me, was diagnosed with glioblastoma a couple of years before my diagnosis. She knew it was a death sentence and was given 18 months to live. Through sheer will, faith, and determination, she survived for 3 years before finally succumbing. Throughout this time, she continued to enter 5K’s and complete them, even when having to use a cane. I ran with her numerous times throughout this period. My first call after getting my diagnosis was to Julie, as I knew she’d have the right words to say. Her story gave me the courage to face my disease with the same strength.
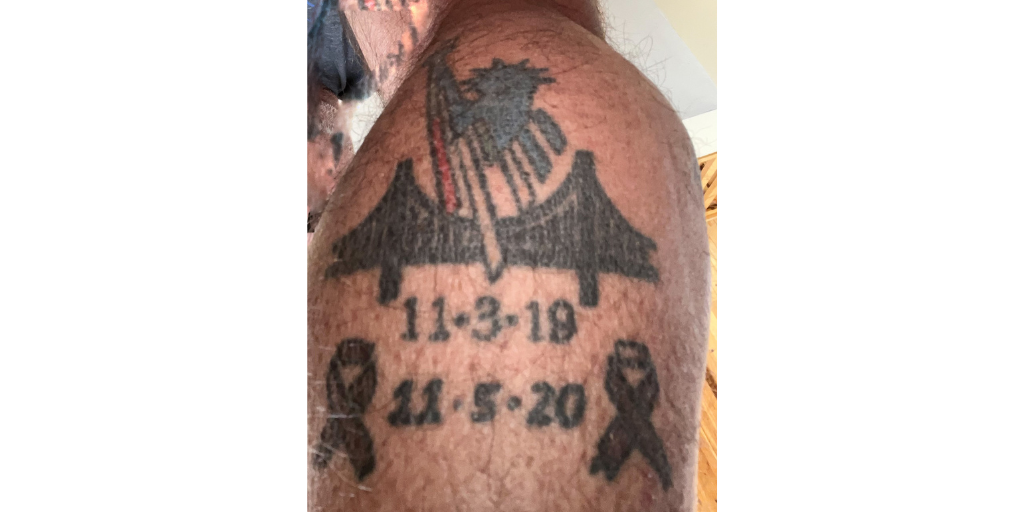
Two quotes give me strength. I wear a bracelet with a metal tag that a friend gave me a few days after my SCT while I was still in the hospital. It says, “Stronger than yesterday.” I’ve only taken it off once in almost 4 years! I tag all my runs with “#strongerthanyesterday.” The other quote is “No Limits.” I borrowed this one from Pat’s Run, a local run in honor of Pat Tillman, a former Arizona State University (my alma mater) and Arizona Cardinals football player who gave up an NFL career to serve his country. Sadly, he was KIA in Afghanistan. I’ve participated in the run for 9 consecutive years, including virtually during COVID. This mantra means so much to me that I got it tattooed on my left calf.
See link to a story that my running coach published to her social media accounts.
The MMRF is delighted to recognize Marc Schiff as the MMRF Spirit of Hope Honoree at the 2024 MMRF Team for Cures: Scottsdale Walk/Run. Donate to his team “Runners & Walkers United” to accelerate a cure!
This award is presented at every Walk/Run to a patient, caregiver, or family who inspires hope through their resilience, perseverance, and dedication to the MMRF and its mission.